After a sexual assault, the survivor may choose to go to the emergency room for evaluation. The experience survivors go through when being examined after a sexual assault is both physically draining and emotionally taxing. Even when every precaution is taken to avoid re-traumatizing the survivor, the experience remains intrusive and deeply personal.
MultiCare Auburn Medical Center (MAMC), ER Physician Dr. Java Tunson, shared that many survivors may come to the ER for reasons other than sexual assault. The survivor could be in a domestic violence situation and be utilizing other medical reasons to seek out treatment. A survivor may also come in for a reason that has nothing to do with sexual assault. Using both medical training and intuition, medical staff must discern the underlying cause and ensure to provide necessary treatment.
Treating Sexual Assault Survivors in the ER
Every patient that comes to the ER is triaged by one of the hospital’s nurses. This brief intake is done with every patient, at every ER. In triage, the nurse collects necessary, vital, medical information for the ER staff. The patient is then assigned a room in the ER for further treatment after triage.

Some hospitals have a Sexual Assault Response Team (SART) room available in their ER. This room is often designed to have less of a hospital feel for the comfort of the survivor. This room is private and usually apart from the disruptive din of the ER. MAMC does not have a SART room. However, since the ER’s renovation, all ER patient rooms are private and lock.
MAMC has a pool of Sexual Assault Nurse Examiners (SANE) available to call when a survivor comes to the ER for care. These specially trained nurses are available to multiple sites and are always on call. Once requested they come to the ER. The SANE is paged as soon as the survivor is triaged, as it can take up to an average of 30 to 45 minutes for the SANE to arrive. Some of MAMC’s nurses are also dual trained.
The exception to this is that when a child is brought in with suspicion of sexual assault or abuse. Dr. Tunson explained that after the same stabilization measures for adults are taken, the child is transferred to Children’s Hospital for a pediatric SANE evaluation. Once transferred, possible admission until safe disposition is determined may occur.
According to Makenzy Byrum a SANE with Rapid Sexual Assault Victim Exam (SAVE) Investigation, LLC, a SANE “typically responds to sexual assault patients in the ER or community settings like [a] detention center or university health centers. We are responsible for the head to toe examination of sexual assault patients and forensic evidence collection. We also work with patients in discharge planning, make referrals for community resources and help make recommendations for STI [prevention] and emergency contraception. Outside of the clinical setting, we are also involved in courtroom testimony should the case go to court.”
SANEs are registered nurses with advanced training in forensic evidence collection. These nurses go through 40-hour didactic training to learn how to conduct an effective sexual assault exam and work as a member of a SART. SANEs also receive clinical training with a speculum and additional clinical training including multiple precepted forensic exams with an experienced SANE or physician. Locally, further education experience is available for SANEs by touring the WSP crime lab, meetings with the Sexual Assault Center of Pierce County (SACPC) and King County Sexual Assault Resource Center (KCSARC) and through courses taught at Harborview.
Dr. Tunson explained that when evaluating a presenting survivor, they first ensure there are no physical injuries that require stabilization. Some injuries doctors look for are brain bleeds and profuse vaginal or rectal bleeding. “We try to spare [the survivor] a pelvic exam if no symptoms are present to necessitate it.”
 When examining the survivor, the physician’s role is to talk with the patient and determine any injuries. While they review what happened briefly, the medical staff does not delve into the legality of the assault. Physicians must reassure that the survivor is not physically injured, while social workers address the immediate mental aspect of the assault.
When examining the survivor, the physician’s role is to talk with the patient and determine any injuries. While they review what happened briefly, the medical staff does not delve into the legality of the assault. Physicians must reassure that the survivor is not physically injured, while social workers address the immediate mental aspect of the assault.
When treating survivors, Dr. Tunson explained, the medical staff tries to clarify all the medical staff’s roles, so the survivors aren’t reliving the trauma. Working with effective communication between the teams is a critical role in ensuring this. She shared that interacting with a patient who has just experienced an assault is “heartbreaking. It’s terrible. Even coming forward is courageous and difficult.” Dr. Tunson continued that “[in the ER] we experience a lot of people that feel shame for the assault, even though it has nothing to do with them.”
Administering the Sexual Assault Victim Exam
After a physician ensures the survivor does not require immediate medical intervention, a forensic Sexual Assault Victim Exam (SAVE) is offered. At MAMC, this exam is only performed by a SANE. This exam is entirely up to the survivor and is never forced or coerced.
If the survivor chooses to have a SAVE, only those individuals necessary, including a trained advocate if requested, are present during the exam. While some survivors come to the ER with a tribe of supporters, their privacy and safety are paramount. Medical staff may request those accompanying a survivor to wait until after the exam for the survivor’s comfort.
Before a SAVE is performed, the SANE talks with the survivor about what to expect during the exam. The SANE reviews what parts of the body will be examined, and how. If the survivor wishes only part of the SAVE, only that portion is completed. Though a SAVE will still be performed, evidence collection is limited to the time frame of typically 120hrs – or 5 days post-assault.
The first part of the SAVE is collecting information. The SANE gathers routine medical information, as well as a history of the assault, documenting the assault in the survivor’s own. The SANE will ask what the survivor recalls, if the assailant is known to them and what parts of the body have been impacted. Having this information “helps know what is to be examined and where to collect from,” explained Byrum.
Once this information is gathered from the survivor, the head to toe examination is performed. This portion of the exam may be based on this survivor’s experience and the provided history. On average, the exam takes approximately two hours, but depending on the severity of injury, some exams can take four to six hours. The survivor’s body remains covered until that portion is needed for examination. Every step of the exam is explained to the survivor as it is performed. Before touching the survivor, the SANE reviews what will happen next.
The Careful Examination of a Sexual Assault Survivor
Consent for the SAVE is a continuous process. If at any point the survivor requests the exam to stop, it does. If the survivor requires a break, the exam ends until the survivor can continue. The survivor is reminded throughout the process that they can stop at any time.
If the survivor came to the ER in the clothing they wore at the time of the assault; all these items are collected – including the survivor’s undergarments. The survivor is, however, under no obligation to turn over their clothing for evidence. Each article of clothing is separately packaged as evidence. It is also at this time that any loose debris, such as grass or dirt, that may have come from the assault site is also collected.
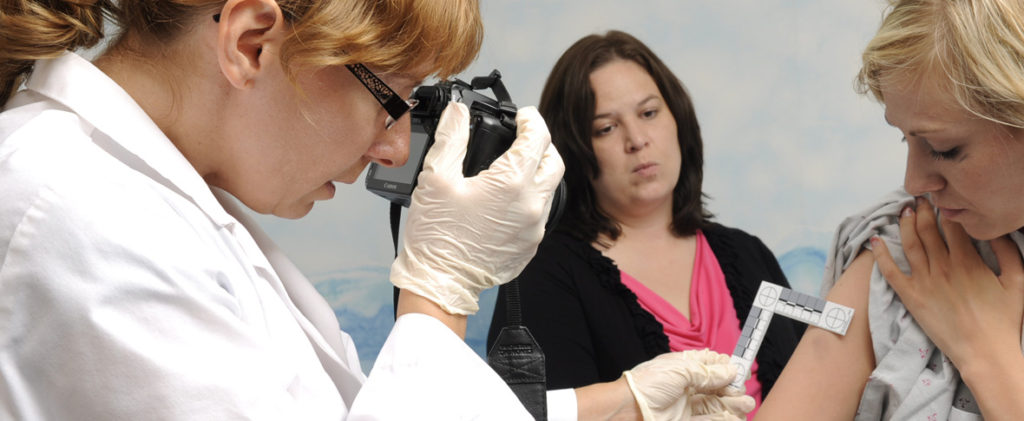
First, the SANE will photo document any non-genital injuries on the survivor’s body. Several head hair samples are taken. Multiple oral swabs are done, getting saliva samples. Swabs of the hands and from beneath the survivor’s fingernails are collected. Skin swabs are taken from throughout the body to gather any potential trace evidence. The SANE takes meticulous care when collecting samples from the survivor throughout the exam.
To collect genital evidence, the SANE will first examine for visual signs of trauma before any swab collection is done. Pubic hair combings and collection is done. Multiple swabs are taken from the perineum, vaginal, penile and scrotal regions. After a vaginal exam may be performed using a speculum, cervical swabs are taken. Anal swabs are taken if any penetration occurred during the assault. Rectal swabs, which differ from anal swabs, are not routinely collected.
Any foreign bodies found in the survivor’s vagina or rectum during the examination are removed and collected as evidence.
Blood and urine samples are also taken from the survivor. If the survivor was drugged or shows signs of drugging, toxicology testing is done on these samples. All blood and urine samples are sent with law enforcement for toxicology processing at the WSP crime lab. According to the FDA, Benzodiazepines (such as Rohypnol and Temazepam) can present in drug tests up to 1-4 days after consumption.
Medical Consequences of Sexual Assault
At the end of the physical exam, the SANE will discuss recommendations for STI preventatives and emergency contraception. It is entirely the choice of the survivors what, if any, medical interventions they take post-assault. STI prophylaxis is a one-time dose of multiple medications in the Emergency Department. HIV prophylaxis is a 28-day dosing, generally with repeat testing done at 6 months.
Each year, an estimated 25,000 American women will become pregnant following an act of sexual violence. As many as 22,000 of those pregnancies could be prevented through the prompt use of emergency contraception.
Dr. Tunson explained that HIV prophylaxis, which patients are on for months, have long-term side effects such as nausea and other flu-like symptoms. Patients who decide against prophylaxis may instead get a large dose of antibiotics. This has potential side effects of cramping, stomach pains, and diarrhea. Patients who utilize an emergency contraception pill may experience vaginal bleeding, cramping or alterations in mood.
Survivors may also experience medical impacts beyond the side effects of prescriptions utilized after an assault. Some survivors have lacerations, and though less likely, may have trauma requiring surgical intervention. Dr. Tunson also explained that survivors might experience long-term side effects from pelvic or genital trauma because of the assault. It is far more common that no physical injury is present.
What is more prevalent is the psychological impact on survivors. Both in the immediate aftermath and in the months after, survivors often show symptoms of “PTSD, depression, and anxiety,” said Dr. Tunson.
It is because of this the SANE will arm survivors with aftercare resources before they leave. Community resources such as KCSARC or SACPC are available to survivors for counseling and advocacy. Follow up medical care is also discussed with the survivor.
Choosing to Report
If the survivor wishes to report the sexual assault to the police, the SANE will help facilitate that process. Just as a SAVE is not mandatory, a survivor has no obligation to report or give a statement about their sexual assault to law enforcement. Having a SAVE does not require a survivor to report their sexual assault. The exception to this is the sexual assault of children and vulnerable adults, as medical staff are mandatory reporters.
Once a sexual assault has been reported to law enforcement, the evidence collected is turned over to the police. This maintains the chain of custody. This evidence – what is most often referred to as a rape kit – will then be sent to the WSP Forensic Crime Lab for testing.

If the survivor has a SAVE performed but does not wish to report to law enforcement the hospital will store the kit. Each hospital has a different policy as to the length of time they will hold these kits, and how they contact survivors before destroying unclaimed kits. For MAMC, and all of Puget Sound, kits for survivors who do not wish to report their sexual assault are held for a minimum of 60 days.
Dr. Tunson said she was not sure if there is more sexual assault or if there is more discussion or awareness that makes it seem that there is more. For Dr. Tunson, survivors should know that “as a provider, we see it too frequently. Sexual Assault should not be stigmatized. There is no shame.”
Recognizing that anyone can be a victim is imperative. The definition of sexual assault is broad and is not limited to the stereotype of man on woman, vaginal intercourse. Male sexual assault survivors are not rare. In the last six months, Dr. Tunson saw several male survivors and acknowledged that her colleagues had seen several as well. She stressed that female on male sexual assault is very real and is no more shameful than any female survivor’s sexual assault. “It is not for [us] to judge the circumstances of someone having their body violated.”
When asked about false reporting, Dr. Tunson said that it was “not our role to question. Our role is to ensure the patient is safe, not injured and should they want a SANE – they get it. Our role is not forensic or legal. We are not there to determine if it is a false report.”
Preventing Secondary Trauma
To help ensure no secondary trauma occurs while treating survivors of sexual assault, ER staff often depend on peer support. Dr. Tunson shared that “as a profession, we are caretakers and don’t always do a good job taking care ourselves or each other.” But, she continued, “as ER physicians have a higher risk of burnout – we are becoming more aware.”

At MAMC, a program named ‘Code Lavender” has been implemented. This program exists so that medical staff that feel unsafe, are having trouble with a case, are being assaulted, or are having difficulty coping can receive assistance and resources. Staff can call a Code Lavender on a colleague if they feel they need the support. Once a Code Lavender is called, the staff member is followed up with to see if further resources are needed or wanted.
Byrum shared that while there is no formal counseling offered through RSI, peer support is paramount. Coordinators are also available to debrief when necessary. During training and continuing education SANEs are taught by social workers and mental health professionals about the importance of self-care.
One of the most important things Dr. Tunson emphasized was that MAMC “is a safe haven for the community. Anyone who comes in will be taken seriously and offered a sexual assault examiner. We are there 24/7, and anyone can present – it doesn’t matter when. If they have showered, it doesn’t matter. If three days have passed – it doesn’t matter. We are always there. This is a safe place. We do not disclose who is in the ER. If people need help in any way, we are a safe haven. It doesn’t matter who, when or under what circumstances.”
Dr. Tunson received her bachelor’s in health and society/biology from the University of Pennsylvania in 2006 and obtained her Doctor of Medicine from the University of Colorado School of Medicine in 2012. Prior to coming to MAMC in 2016, Dr. Tunson did her residency at Denver Health Emergency Medicine.
Byrum obtained her bachelor’s in nursing from OHSU in 2003 and worked primarily in emergency nursing. In 2005 Byrum became trained as SANE. She is a co-chair of the Multnomah County SART and sits on the Medical Forensic committee for the Oregon Sexual Assault Task Force.












[…] no threat of danger is established, or the threat is removed, the officer will take a report. Commonly officers respond to hospitals, where survivors have just undergone the Sexual Assault Victi…. This report establishes the time and location of the assault and gathers necessary details about […]
[…] processing techs and other staff will hold an “Informational Picket for Quality Care” at MultiCare Auburn Medical Center. Caregivers will be informing patients and neighbors about severe problems with short-staffing, […]
[…] Auburn, WA– On Tuesday, February 12, scores of licensed practical nurses, certified nursing assistants, food and nutrition services workers, ER techs, housekeepers, sterile processing techs and other staff will hold an “Informational Picket for Quality Care” at MultiCare Auburn Medical Center. […]
[…] Finally, the percentages of 8th, 10th, and 12th-grade students who report ever having experienced sexual assault are alarming. In 2018, 36 percent of 12th-grade female students reported having been sexually assaulted. In addition, nearly one-third of 10th and 12th-grade students report having witnessed sexual assault. […]